Truvada as PrEP: A new HIV prevention option on the table for Zimbabwe?
 Opinion Paul Sixpence
Opinion Paul Sixpence
RECENT policy pronouncements by the World Health Organisation (WHO) recommending national public health systems to incorporate Truvada as Pre-Exposure Prophylaxis (PrEP) into their prevention interventions present a new revolution in the fight against new HIV infections. The WHO guidelines came on the background of overwhelming science that proves that Truvada as PrEP works when taken correctly as presented at two major global HIV and Aids conferences namely the 2015 Conference on Retroviruses and Opportunistic Infections (CROI) and the International Aids Society (IAS) 2015.
In light of scientific evidence that proves that PrEP works and considering the burden of HIV and Aids to Zimbabwe’s socio-economic development, this instalment advocates for PrEP roll-out for young women, sex workers and sero-discordant couples in Zimbabwe.
What is PrEP?
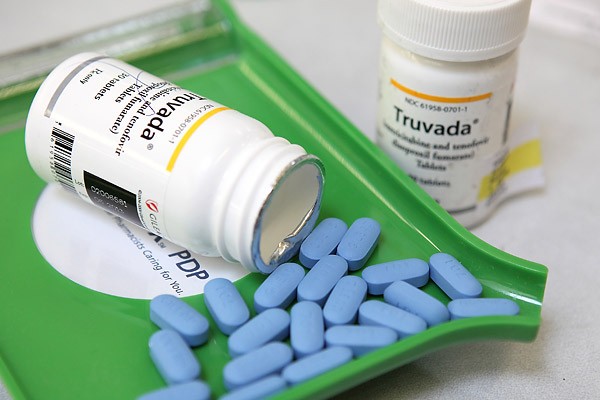
Pre-exposure prophylaxis is the use of antiretroviral medications (ARVs) to reduce the risk of HIV infection in people who are HIV negative. Truvada is an ARV that has been approved in Zimbabwe for treatment purposes. In a nutshell, PrEP is the taking of preventive drugs to prevent primary infection prior to engaging in a potential risky sexual encounter that can possible expose one to HIV infection. In other words, it is akin to taking anti-malaria tablets prior to getting into a malaria zone.
Evidence that proves that PrEP works
This article is based on the TDF2 and Partners PrEP clinical trials. TDF2 was conducted in Botswana among young heterosexual couples and Partners PrEP was conducted among sero-discordant couples in Kenya and Uganda. Both clinical trials exhibited efficacy rates of over 80 percent.
PrEP efficacy and feasibility case studies presented in this piece have been deliberately chosen because they were conducted in Africa and in resource constrained settings relatively similar to those obtaining in Zimbabwe. There are other clinical trials that have been conducted in France, Britain, Brazil and the United States of America, among diverse sets of population and they all indicate that PrEP works.
Taking note of all these positive and inspiring findings in the field of HIV biomedical interventions, the president of the International Aids Society and Chair of IAS 2015, Chris Beyrer had this to say:
“The science on PrEP is overwhelming and its conclusions are clear: PrEP works when taken. Access to PrEP is now a public health and human rights imperative. The studies presented here [at IAS 2015] provide the most detailed data to date on PrEP implementation successes and challenges, underscoring that the intervention is feasible and effective in the real world. We hope these studies launch the beginning of a new PrEP era.”
Current global trends in adopting PrEP
PrEP was licensed for treatment purposes in the United States of America in July 2012. Applications for regulatory approval have been filed in Australia, Brazil, Canada, South Africa and Thailand.
Is PrEP for Zimbabwe?
PrEP is not for everyone but for specific populations at high risk of infection. Among those who are in need of PrEP in Zimbabwe are key populations, namely, young women, sero-discordant couples and sex workers.
Presenting oral evidence to the Parliament of Zimbabwe Thematic Committee on HIV and Aids in July 2015, National Aids Council (Nac) Chief Operations Officer, told the Committee that his organisation was worried about the increasing rates of new infections among girls and young women between the ages of 15 and 24 years.
He noted that about 80,000 young girls and women were living with HIV as compared to 36,000 of their male counterparts. These statistics speak of an urgent need to offer young women with a wide range of HIV prevention options.
According to the Centre for Sexual Health and HIV/ Aids Research (Ceshhar) out of 52,214 sex workers almost 11,000 (20 percent) are living with HIV. These figures speak of an urgent need to provide sex workers with new and effective solutions in preventing primary HIV infection in addition to messages on correct and consistent use of condoms and behaviour change.
The way forward
There is an urgent need for collaborative engagement between policy makers in relevant State institutions, HIV and Aids researchers and civil society actors to analyse the science that proves that PrEP works with the local context in mind, work on regulatory approval, develop guidelines and roll-out PrEP to those at high risk of HIV infection and who need it.
From November 29 to December 4, 2015, Zimbabwe will host the International Conference on Aids and STIs in Africa (ICASA).
In light of the encouraging PrEP efficacy and feasibility results, ICASA 2015, should serve as a marketplace of ideas and exchange of knowledge on how to mobilise resources for PrEP roll-out, enhancing the capacity of public health systems to integrate PrEP into their existing comprehensive HIV treatment and prevention packages and ways of raising awareness among people of the existence of this new HIV prevention option.
Paul Sixpence is an HIV prevention and treatment advocate. He can be contacted on: [email protected]










Comments