WATCH: Modern, painless surgeries for women at UBH

Thandeka Moyo-Ndlovu, Senior Health Reporter
WOMEN in the southern region will now have access to painless, scar-free specialised gynaecological surgeries which will help address the prevalence of reproductive health challenges like fibroids, hysterectomy, ectopic pregnancies, early-stage cancers and infertility.
The procedure, VNOTES (vaginal natural orifice transluminal endoscopic surgery) will be accessible at the United Bulawayo Hospitals (UBH).
UBH will also offer laparoscopy – a type of surgical procedure that allows a surgeon to access the inside of the abdomen (tummy) and pelvis without having to make large incisions in the skin. This procedure is also known as keyhole surgery or minimally invasive surgery.
Patients who access these internationally recommended specialised surgeries need minimal painkillers as they recover quicker than those who use traditional methods where surgeons make large cuts on one’s abdomen to access the womb.
The procedures were first introduced on Monday at UBH by a team of renowned local gynaecologists led by a New Zealand-based Zimbabwean urogynaecologist Dr Elliot Mackenzie, who specialises in female pelvic medicine and reconstructive surgery.
Dr Mackenzie, who brought in some of the equipment from New Zealand, will be helping specialists at UBH familiarise themselves with the advanced procedures for the rest of this week.
In an interview yesterday, Dr Mackenzie said he was happy to conduct such surgeries at UBH where he did his housemanship before moving to New Zealand.
He said the first patient who had a hysterectomy – a procedure to remove her womb through VNOTES – was up and running within 12 hours after surgery.
“I was invited by my local colleagues, obstetricians and gynaecologists working in Zimbabwe so that we can share knowledge and skills since I work in New Zealand where I am based. I do dedicate part of my holiday to doing surgical camps, lectures, etc. and this time we decided to operate so that we share knowledge on new approaches being used in first world countries like New Zealand,” said Dr Mackenzie.
“What we have recently started doing is hysterectomies through the vagina by using laparoscopic equipment and this is such that at the end of the day the patient doesn’t have scars on the abdomen and the surgery is almost painless. We also know that our patients require minimal painkillers as opposed to the traditional methods.”
He said patients who undergo such procedures heal quicker than they would if they had the traditional standard approaches.
“The reason most patients have pain is that traditional procedures tamper with the abdominal wall and the stitching comes with some pain.
My colleagues indicated that there are small gaps in terms of certain things that they needed to know in order to get started so we are happy to come in and share knowledge so that in a week they are able to roll out these services to women as they are capable.”
Dr Mackenzie said last week he also led a team of gynaecologists at Sally Mugabe Central Hospital in Harare where they conducted surgical camps for women in need.
“We are using VNOTES and we are simply saying there is a way of getting into the abdomen or the pelvis that is already there which is the vagina.
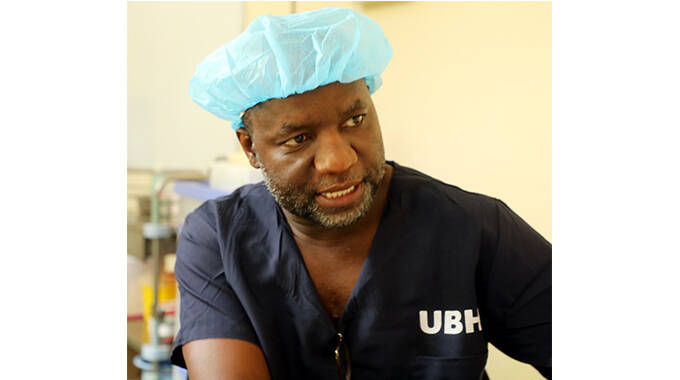
UBH Dr Elliot Mackenzie
Therefore, there is no need to take the abdominal route and make holes there,” he said.
In explaining the procedure, Dr Mackenzie said when operating, surgeons need to get more space to see hence they start by inserting a device that sits on the vagina.
This device traps air, carbon dioxide, which then balloons the abdomen and surgeons then put in cameras and other instruments before operating.
“Women face many problems that arise in the reproductive system, for example problems with bleeding, fibroids, early-stage cancers, endometriosis, sometimes pregnancies may develop outside the womb – what we call ectopic pregnancies. All those prevalent conditions have always been dealt with traditionally, but we now use a less painful procedure,” Dr Mackenzie said.
Dr Mackenzie added that he was happy that Bulawayo, which is like a second home to him, will be able to offer the service which is already being rolled out in developed countries.
“I have a special spot for Bulawayo since I did my housemanship at UBH and Mpilo and my lovely wife is also from the City of Kings. This procedure will also help us access women with infertility challenges as well.
We will make small holes using laparoscopy and we insert a camera to see if the tubes are open or blocked as these are the major reasons why women sometimes fail to conceive. We will then use a device to inject inside the womb to determine the problems,” he added.
A Chronicle news crew caught up with Ms Sakhile Moyo – the first beneficiary – who said the procedure was indeed painless and less hectic.
“I am grateful to these skilled doctors who took their time to help relieve my pain after feeling pain in my womb. I feel strong and was able to walk properly by myself and walk up and down within a few hours. I also urge other women to come forward as these procedures will help us live longer and take care of our families,” she said.
UBH clinical director Dr Harrison Rambanapasi said the introduction of the procedures will help doctors clear waiting lists quicker than before.
He said the hospital is fully booked until December 2023 for hysterectomies and some patients with reproductive system challenges were going to benefit.
The procedures are done at an affordable cost compared to private institutions which normally charge in forex.
Sundries are the only ones pegged in foreign currency, US$20 payable at the prevailing rate, while the rest of the services are pegged in local currency at UBH.

UBH clinical director Dr Rambanepasi
“We hope to achieve more now that we will be rolling out these specialist services at UBH pegged at minimal costs considering that this is a public hospital. Theatre fees will be pegged at $10 000, visualisation of pelvic viscera at $9 056 while laparoscopy will be pegged from $12 424,” said Dr Rambanepasi.
Bulawayo Provincial Affairs and Devolution Minister, Cde Judith Ncube also visited the team of specialists at UBH and commended them for bringing such a great service to the people in Matabeleland.
“We are grateful as women from the southern region and it’s exciting to know there has been advancements in the treatment of reproductive health problems that affect a number of us. We grew up with many women suffering but with this, I am confident that our days of suffering are over.”
Renowned gynaecologist Mr Francis Chiwora, who was part of the team, asked Minister Ncube to help mobilise equipment so that UBH can sustain the project in future.
“We are grateful to Hon Ncube for visiting us and to this young man who came all the way to teach us how to use modern technologies.
He brought some of the equipment from New Zealand and we appeal to Minister Ncube to help us get these items for our public institutions.
So far these services were only at Mater Dei and it is time that we offer them at our public institutions so that the general populace benefits,” said Mr Chiwora. -@thamamoe









Comments